Bone density test results2/27/2023  
A normal T-score is greater than minus 1 (-1), whereas a T-score of minus 1 to minus 2.5 indicates osteopenia, and a score of minus 2.5 or less indicates osteoporosis.Ī Z-score compares your results to other individuals of the same age, weight, ethnicity, and gender. A negative value is an indication of thinner bones with low BMD, and a positive value is an indication of stronger bones. Your T-score will be your BMD compared to the average score of a healthy 30-year-old. Results of a BMD test are reported in two ways as T-scores and as Z-scores. Ideally, it is best to test the same bones (preferably, hip and spine bones) each time with the same BMD technique to achieve reliable results. A DPA scan can take about 30 to 45 minutes to complete the test. The DEXA technique used to scan the hip and lower spine will take about 20 minutes. After the bones are scanned by the machine, the amount of radiation absorbed will be measured. The radiologist will pass a scanner over your body to take X-rays of the bones. You will lie on your back on a padded table. The BMD scan is conducted in a special radiology department. 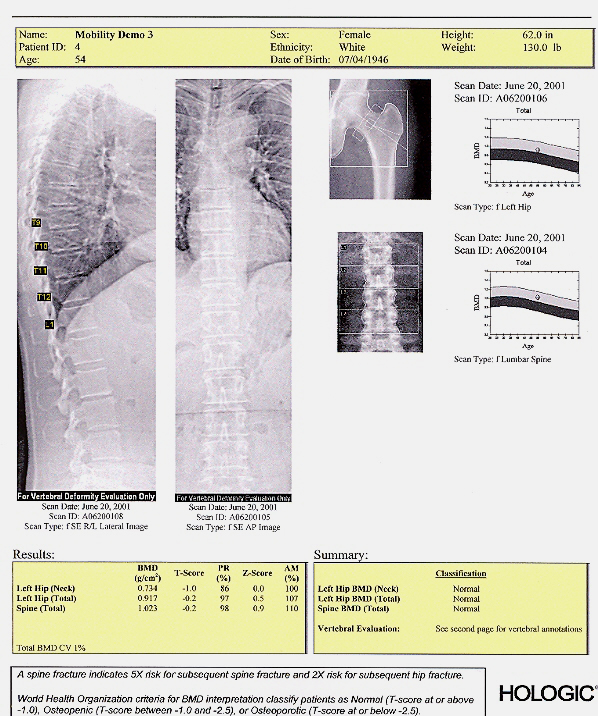
Further testing is required to confirm a diagnosis of osteoporosis. It is often used on the heels as a screening test at health fairs. Ultrasound uses sound waves to measure BMD and is a quick and painless procedure without the use of radiation. P-DEXA is a portable device which gives faster results than DEXA.ĭual photon absorptiometry or DPA uses low dose radiation to measure BMD in the hip and spine region. Peripheral dual-energy X-ray absorptiometry or P-DEXA is a type of DEXA test used to measure BMD in the wrist and forearm or legs. It is the most accurate method of measuring BMD. Long term consumption of corticosteroids.ĭifferent techniques of measuring BMD include:ĭual-Energy X-ray absorptiometry or DEXA uses two different low dose X-ray beams to estimate BMD in the hip and spine region. 
Younger women with increased risk of osteoporosis. This test helps in the diagnosis of osteoporosis, a silent disease that thins and weakens bone and increases the risk of fractures.īone mineral density testing is recommended for the following individuals: If your bones are weakened, you can seek treatment, adjust your diet and exercise, and take all the appropriate measures to minimize your risk of fractures.A bone mineral density or BMD test uses special low dose X-ray to measure the density of calcium and other minerals in your bones to assess bone strength. A DEXA scan could change the trajectory of your life. Strength and weight-bearing exercise is also critical as well as limiting your alcohol and caffeine consumption and cutting out smoking.īe sure to follow bone density scan recommendations. Just as important as medication is a well-balanced diet with sufficient calcium and vitamin D (if you’re not getting enough of these nutrients in the foods you eat, your doctor may recommend supplements). Treatment for abnormally weakened bones usually includes medication to slow, stop, or even reverse the process. Researchers believe that the reason for this is that screenings can uncover thinning bones in time for treatment. However, bone density screenings can lower fracture risk by 36 percent, according to one Johns Hopkins study. While more than 50 percent of women and 18 percent of men over the age of 50 have reduced bone mineral density, many don’t know it until they have a fracture, and this condition doubles the risk of a hip fracture. That’s because osteoporosis is a silent disease. Women over 65 (in your 50s, for those who are at high risk) and men over 70 should undergo a bone density screening, even if they’ve never had a fracture. This quick and easy X-ray, called a DEXA scan, measures the mineral content of your spine, hips, and sometimes the forearm and determines if you have reduced bone mass – osteopenia or even osteoporosis. If your physician doesn’t recommend a bone density test after you break a bone, be proactive and request one. Recent studies have shown that men who have experienced a high-trauma fracture were similarly at risk for a later fracture. Crandall, an internal medicine physician at U.C.L.A.’s David Geffen School of Medicine, who led the JAMA Internal Medicine study, the same goes for older men. As expected, those women who had broken a bone in a minor accident had a 52 percent greater risk of recurrence, but even those women who had experienced a fracture in a traumatic accident were 25 percent more likely to break another bone compared to their peers who hadn’t experienced that first fracture.Īccording to Dr. For eight years, the study followed a group of 7,000+ postmenopausal women (many in their 50s and 60s) who had sustained a fracture. 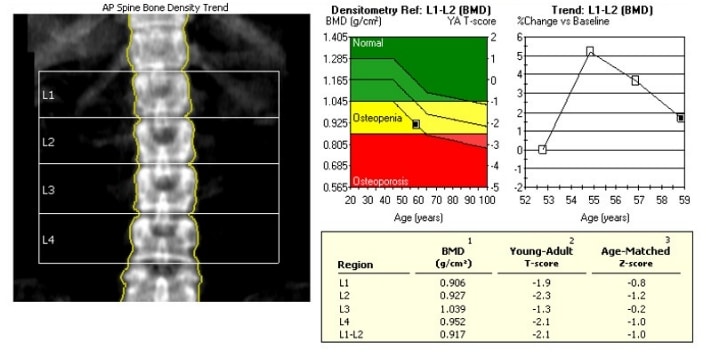
Consider a recent study published by JAMA Internal Medicine. There’s growing evidence that anytime a post-menopausal woman or man over 70 breaks a bone – no matter what the cause – it’s a red flag. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
